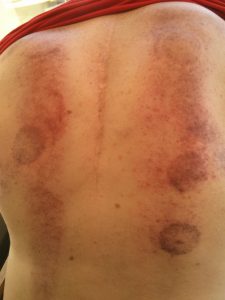
Chronic Pain Management
On September 11, 2009, I broke my spine, leg, ankle and collarbone, bruised my heart, as well as fracturing my sternum and ribs, and my head split open. Although I don’t remember this, the only complaint I had a few minutes after the accident, was the pushing of towels on my head, to stop the bleeding. For the next year, I experienced minor pain and had no need for chronic pain management until October 2010. The chronic pain commenced when I woke up and started shouting
“help me”, “I need help”, “I am dying.”
I grabbed the nurse’s call bell and kept on pressing it. Similar to people who think that continuing to hit the lift button would get the lift there more quickly. A nurse promptly arrived and with a smile said “Hello John what would you like”, so I repeated it, and louder this time. My pain levels decreased by a small amount after taking a hefty dose of pain relief. I continued to ring the call bell and asked for help. The pain was centred around my level of injury and focused on my sternum all the way through to my back. I felt as if there was a pole stuck through my body.
I was suffering from Syringomyelia, a spinal disorder that I’ve never been able to pronounce. A cyst (or cavity or syrinx) forms within the spinal cord, and it grows more significant over time, destroying the spinal cord. It stretched from T1 to T9, which seems like a long way. The serious condition may result in pain, paralysis, and weakness. It only affects around 1 out of every 10,000 people, and I had three operations to drain the cavity via a series of catheters, tubes, and valves. All of which would remain within my body. The doctor hoped that the cavity was the cause of the pain issues, and once drained the pain would reduce.
Three operations to reduce the pain
Before the first operation, I prayed to God that the pain would disappear, and I woke up in the recovery room, and the pain levels were the same. The next morning a group of about 20 doctors with white coats and clipboards appeared at the end of my bed, and they all looked pleased with themselves. The smiles disappeared when I shared the reality with them. Every year I would have scans of the syrinx to ensure it wasn’t growing. The pain remained with me and is my number one health issue. On a scale of 1 to 10, my base rate of pain is 5/10. It increases during the day and resets after 8 hours on my back in bed overnight. I have concerns that the “reset” will stop one day. As the day passes the pain level increases and typically I go to bed when it reaches 7/10. When it gets to 9/10 I call for an ambulance, and the officers cannot offer me anything that I haven’t already taken, and I go to the hospital.
There is a slight chance the pain is brought on by the metalwork that was placed on my back to support my spine, and he could operate to remove it. We decided against this, as the operation was risky and the success rate was low. Chronic pain management is vital to my life, and the first method of dealing with my pain was drugs.
Chronic Pain Management tip 1. Pain Relief Medication
From the time the chronic pain commenced, I was taking large doses of pain relief, as often as I was legally permitted to do so. I had too. Each day I was taking 80 mg of immediate pain relief, 120 mg of long-term pain relief, and 600mg of Lyrica (nerve pain relief). The first two are opioid pain medications and often called narcotics, with a long list of possible side effects including constipation and fatigue. Following a few years of being on the maximum pain relief possible, I was encouraged by my partner Madie, to reduce the levels. She mentioned that people waiting to die have similar levels to enhance their life just before death. As I wasn’t preparing to depart Earth, I reduced the levels. My doctor advised to slowly reduce the levels of opioids, as he wanted to ensure I could manage increased pain and the withdrawal which would occur as I was hooked on the drugs.
I knew of the experience of drug withdrawals from the time I forgot to visit my pharmacy a few months after I arrived home from the hospital. It was a long weekend, and I managed to cope with one day without the pain relief, but after hitting the 2nd day I became anxious and then angry. I couldn’t stop moving my arms around, and the anger made me throw things around the room including a coffee cup that exploded into pieces after hitting the wall. Eventually, I managed to reduce my daily intake of long-term pain relief from 120mg to 30mg, without any increase in pain.
Chronic Pain Management tip 2. Self-Hypnosis
I imagined hypnosis to be the fake entertainer that took people from the audience, who were paid actors to do what the magician on stage told them. So when a psychologist trained me to perform hypnosis on myself, I was sceptical. After a few lessons I believed in self-hypnosis, and apart from the process involves breathing, I won’t go into more details here. The goal is to take the focus away from the pain and onto something else. The “something else” for me is to be busy doing enjoyable and positive things which takes the focus off the pain. Many times the pain disappears until someone asks about it, or the pain levels get too high.
Chronic Pain Management tip 3. Exercise
When you are experiencing chronic pain, it seems logical that avoiding exercise is a good idea as it may increase the pain. For myself, the opposite is true. During the workout I no longer notice my back pain, and I think it is a combination of 1) exercise causes pain in other areas and 2) the pain in my back decreases. Following exercise, the pain levels drop, and I feel better, both physically and mentally. However, it makes my arms sore. The best workout for me is Immersion Therapy with Determined2. The endorphins released by the body during exercise are the key. As I am sitting down between four and twelves hours a day, it is vital to move my body around, and it includes… lifting my bottom off the cushion; leaning back in the chair and lifting my legs to my nose; putting my legs on opposite leg; touching my toes; neck exercises; reaching backwards each side. I hardly use my manual chair, as I see many older wheelchair-bound people with shoulder issues, and use exercise instead.
Chronic Pain Management tip 4. Staying Positive
It is easy to focus on my disability and the things I cannot do. I focus on what I can do, and try to do better than people without a limitation. e.g. swimming a kilometre, or managing a book project. It is vital to have contact with positive people and to remove the negative ones from your life. They drag people down to their level. Having a Faith helps me, and I worship and serve at Rise Church in Lightsview, Adelaide, as well as communicate and meet with believers at other times. I read books, and in the process of writing my autobiography “Alive and not Kicking”. Stress and anger increase pain, so please try to stay clear of these.
Chronic Pain Management tip 5. Therapies
Voula is my remedial massage therapist, as well as an amateur psychologist, as we talk about life while my muscles are getting treatment. Exercise and poor posture affect my muscles, and the massage helps loosen my body. I’ve also tried cupping and acupuncture, and believe they have improved my health. I attend a physiotherapist who helps with my golf elbow.
Chronic pain is my number one issue, and my approach is to take pain relief while attempting to reduce the dosage. As well as using self-hypnosis, exercise, being positive and trying other therapies.
Chronic Pain Management tip 6. Prayer
Last but not least, prayer is helpful. So far the pain hasn’t disappeared, but I have hope that one day it will. I read about the miracles of Jesus, and that Jesus is the same today as yesterday, so I believe that miracles can still occur.
How do you cope with pain?
Click here for a blog about Biblical Pain. Did Jesus and the disciples experience pain?